Executive Summary
It’s Tuesday morning. Your denial team pulls the root cause analysis on last week’s $847K in claim rejections. They filter for “coverage not in effect” and “patient ineligible” denials. The number: 287 claims. That’s $847K sitting in pending because somewhere along the line, someone verified coverage and got it wrong.
Here’s the frustrating part: you know exactly what happened. Your billing staff checked insurance at appointment time. The patient said they had a Blue Cross. Your IVR system is active. So the claim went out. But what your IVR didn’t catch, and what your staff didn’t have time to manually verify, was that the patient’s Blue Cross plan changed effective 10 days ago. Or the deductible was different than what you assumed. Or there was a prior authorization requirement your system didn’t flag.
It’s Tuesday morning. Your denial team pulls the root cause analysis on last week’s $847K in claim rejections. They filter for “coverage not in effect” and “patient ineligible” denials. The number: 287 claims. That’s $847K sitting in pending because somewhere along the line, someone verified coverage and got it wrong.
Here’s the frustrating part: you know exactly what happened. Your billing staff checked insurance at appointment time. The patient said they had a Blue Cross. Your IVR system is active. So the claim went out. But what your IVR didn’t catch, and what your staff didn’t have time to manually verify, was that the patient’s Blue Cross plan changed effective 10 days ago. Or the deductible was different than what you assumed. Or there was a prior authorization requirement your system didn’t flag.
Insurance eligibility verification errors don’t feel like a big deal in isolation. One claim gets caught, you rework it, move on. But at scale? At a 1,000-bed hospital processing 4,000-5,000 claims per week? These errors are silently eating 2-3% of your gross revenue.
The question isn’t whether you have insurance eligibility verification errors. The question is: how much are they costing you, and why are you still fixing them manually?
The real cost of eligibility verification errors
Let’s start with what eligibility errors actually look like in practice, and why they’re so expensive to fix.
An eligibility verification error happens when your billing system records incomplete or inaccurate information about a patient’s insurance coverage. This includes:
- Patient has coverage, but you recorded the wrong policy number (leading to claim rejection)
- Patient’s coverage was active when you verified it, but coverage lapsed before claim submission (usually 3-7 days later)
- You verified coverage for one plan, but patient actually has multiple plans and didn’t disclose secondary coverage
- Plan had a deductible or prior authorization requirement you didn’t capture during verification
- Coverage verification was done during pre-registration, but coverage changed between pre-reg and date of service
- You verified coverage with the plan, but submitted to a different plan code or network (claims go to wrong payer)
- Patient enrolled in Medicare Advantage mid-year, but your system still shows traditional Medicare
These aren’t rare edge cases. They happen constantly. And each one costs you.
The immediate cost
When a claim denies due to eligibility error:
- 30-45 minutes of rework per claim (re-verify, resubmit, follow up)
- That’s roughly $40-$60 per claim in labor cost (at fully loaded $55/hour billing specialist rate)
- Average rework denial takes 15-21 days to resolve (vs. 5-7 days for a clean claim)
- During that 15-21 day gap, the claim ages in AR, cash flow delays, your DSO creeps up
So a single $2,500 claim that denies due to eligibility error costs you:
- $50 in immediate rework labor
- $2,500 in delayed cash flow (cost of money for 10+ additional days)
- Potential write-off if patient responsibility determination gets muddled
The hidden cost
Here’s what most CFOs miss: eligibility errors don’t stay isolated.
When you rework one claim, you often end up reworking related claims. You discover the eligibility error two weeks after the original claim went out, but by then the patient may have had 3-4 other visits. You have to trace back, re-verify coverage retroactively, and rework everything.
Example: Patient had 6 claims in a month. Your staff verified coverage once at the first visit, recorded it, and used that information for all 6 claims. But coverage lapsed on day 15. Claims 4, 5, and 6 deny. You don’t catch the coverage lapse until the denial comes in (day 21). Now you’re reworking 3 claims, not 1.
The cost of that eligibility error just tripled.
The systemic cost
At a 1,000-bed hospital processing roughly 4,500 claims per week:
- Conservative estimate: 3-5% of claims have some eligibility discrepancy
- That’s 135-225 claims per week with eligibility issues
- Even if only 50% of those end up as hard denials, you’re looking at 67-112 denied claims per week
- 67 claims × $2,500 average claim size = $167,500 per week in claim denials
- Annualized: that’s $8.7M in preventable claim denials
Now, not all of that is total loss. You’ll recover maybe 60-70% through rework. But the remaining 30-40% becomes denial write-offs, extended AR aging, and frustrated patients who get surprise bills.
Even if your actual number is half of that (hospital size, payer mix, claims complexity varies), you’re still looking at $2-4M annually in preventable revenue loss.
What most hospitals do (and why it doesn’t work)
Before we talk about how to fix this, let’s acknowledge what most revenue cycle teams try:
Approach 1: Hire more verification staff
The logic seems sound: if eligibility errors are happening, hire people to do more verification, more frequently. Some hospitals create a dedicated “eligibility verification team” separate from billing.
Here’s the problem: eligibility verification is cognitively draining work. Your staff can manually verify maybe 15-20 insurance plans per hour. At a hospital processing 4,500 claims per week, that’s roughly 900 claim verifications needed. At 20 verifications per hour, that’s 45 billable hours per week just to verify all coverage.
But you can’t verify every claim at the point of service. Pre-registration happens days or weeks before the visit. So you verify again at check-in. Then again before claim submission. Now you’re verifying the same patient 2-3 times.
The real problem: human verification is slow, duplicative, and prone to error. Your staff might verify coverage correctly on Monday, but the data entry is wrong. Or they verify coverage but don’t check for authorization requirements. Or they verify, but the insurance company’s phone system timed out and gave bad information.
You’ve hired more people to do the same broken process faster. The error rate might drop 5-10%, but you’ve added $200K+ in annual labor costs. Your CFO will ask: “Why did we hire 4 people and only improve our clean claim rate by 1 percentage point?”
Approach 2: Implement a new rcm software system
Hospital leadership decides the problem is technology. You implement a “better” RCM system with improved eligibility workflow features. The vendor promises real-time eligibility checks, automated coverage alerts, and integrated authorization workflows.
What actually happens: you spend 5-6 months in implementation. Your team configures eligibility rules. You go live. The system works… the same way your old system worked, just with a nicer interface.
The real problem wasn’t the tool. The real problem was that you were only verifying coverage once (or twice), at the wrong time, and you weren’t checking for dynamic changes (authorization requirements, coverage lapses, plan changes).
New software doesn’t fix broken eligibility timing or incomplete verification logic.
Approach 3: Tighten up your processes
Your COO mandates that every claim must have eligibility verified within 48 hours of submission. Your RCM director creates a new workflow checklist. Your team starts verifying eligibility manually before every claim submission.
This works for maybe 4 weeks. Then your team gets overwhelmed. They start taking shortcuts. They verify coverage but don’t check for authorization requirements. They verify coverage once and assume it’s still accurate a week later when they submit.
Process tightening requires constant enforcement and burns out your team. It’s sustainable for maybe 30 days before it decays.
The real issue: You’re verifying at the wrong time, with the wrong method
Here’s what most hospitals don’t realize: the problem isn’t that your staff aren’t trying hard enough. The problem is structural:
- You’re only verifying coverage at appointment time or pre-registration (sometimes 1-2 weeks before the visit). But insurance changes all the time. Coverage lapses. Plans change. Deductibles reset. By the time you submit the claim, the coverage information is stale.
- You’re relying on IVR systems and manual calls to verify coverage. IVRs are notoriously unreliable (they time out, give conflicting information, don’t capture authorization requirements). Manual verification is slow and error-prone.
- You’re not capturing the full picture of coverage. You check “is this patient covered?” but you don’t check “does this plan have prior authorization for this procedure?” or “is this an in-network provider?” or “what’s the patient’s actual responsibility?”
- You’re verifying at the point of service, but you’re not reverifying before claim submission. Coverage may have changed in the 3-7 days between appointment and billing.
You can’t solve this by hiring more staff or tightening processes. You need to change when and how you verify.
Automated insurance verification: Why it actually works
This is where automated insurance verification changes the game.
When I say “automated,” I don’t mean a bot that checks a single payer database once and says “yep, covered.” I mean a system that:
- Verifies coverage in real-time against actual payer systems (not cached data)
- Checks for authorization requirements, not just eligibility
- Captures complete coverage information (deductible, copay, coinsurance, out-of-pocket max)
- Can be executed at multiple touchpoints (pre-registration, appointment, claim submission)
- Logs every verification attempt so you have an audit trail
- Flags discrepancies and changes in real-time
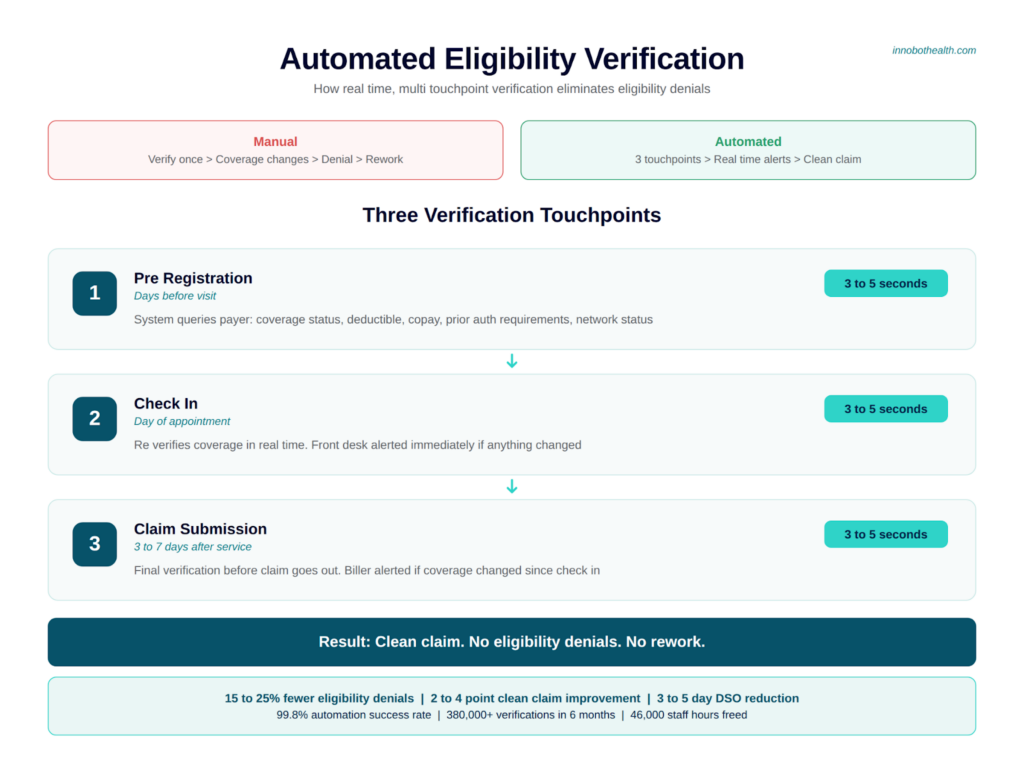
The mechanics: How automated eligibility actually works
Here’s how it works in practice:
The patient schedules an appointment. Your pre-registration system triggers an automated eligibility check. The system sends a real-time eligibility request to the insurance company’s system (through a direct connection or through an intermediary payer platform). The payer responds with:
- Active coverage status
- Effective dates
- Deductible met/remaining
- Copay/coinsurance amounts
- Prior authorization requirements for the patient’s planned procedure
- Network status
- Any plan changes effective in the next 30 days
This happens in 3-5 seconds. No phone calls. No IVR timeouts. No guesswork.
Your system logs this data. If coverage lapses or changes before the claim is submitted, the system alerts your billing team. Coverage is reverified at claim submission time (another 3-5 seconds). If eligibility has changed, your system flags it before the claim ever goes out.
The patient arrives for their appointment. Your check-in system shows real-time coverage status. If the patient’s coverage has changed, your front desk knows immediately and can collect appropriate patient responsibility upfront.
The claim is submitted. Because you’ve verified coverage at pre-registration, appointment time, and submission time, and you have complete authorization information, the claim is built correctly.
Result: claim goes out clean. No eligibility denials. No rework.
What this solves
Automated eligibility verification eliminates the most common causes of eligibility-related denials:
- Coverage lapses between verification and claim submission: Solved. You reverify at submission time.
- Wrong information in your system due to data entry errors: Solved. You’re pulling from the source (the payer) not from what someone typed into your system.
- Missing authorization requirements: Solved. You capture the full coverage picture, not just “is this covered?”
- Claims submitted to wrong payer due to coverage mismatches: Solved. You know the correct primary/secondary payer before the claim goes out.
- Patient responsibility uncertainty: Solved. You know the exact copay/coinsurance/deductible before the patient arrives.
The numbers
Real-world example: Aqua Derm implemented automated eligibility verification with Innobot. They automated 380,000+ eligibility checks in 6 months. They recovered $1.16M that was previously sitting in eligibility-related denial queues. They freed up 46,000 hours of staff time that was previously spent on manual verification and rework.
That’s not theoretical. That’s what happens when you stop verifying coverage manually and start doing it in real-time, at scale.
More broadly:
- Hospitals implementing automated eligibility typically see 15-25% reduction in eligibility-related denials within 3 months
- Clean claim rate improves by 2-4 percentage points (primarily from eliminated eligibility denials)
- Days in AR drops by 3-5 days (because rework cycle accelerates)
- Staff can handle 40-50% more claims with the same headcount (because they’re not spending time manually verifying)
The insurance eligibility verification software decision framework
If you’re considering automated eligibility verification, here’s what to evaluate:
What type of automation do you need?
Not all automated eligibility tools are the same. You have a few options:
Option 1: Basic eligibility checker
A tool that checks “is this patient covered?” It connects to a payer database and returns active/inactive status. This is useful for pre-registration gatekeeping, but it’s incomplete. It doesn’t capture authorization requirements, deductible status, or coverage changes. It’s the minimum viable automation.
Use case: You just need to know if someone has active coverage so you don’t schedule uninsured patients.
Limitation: This doesn’t solve eligibility-related denials because you’re only checking one piece of coverage information.
Option 2: Comprehensive eligibility verification
A system that verifies full coverage details: eligibility status, deductible, copay, coinsurance, authorization requirements, network status, secondary insurance. It’s integrated with your EMR or RCM system so the data flows into your billing workflow automatically.
Use case: You want to eliminate eligibility denials and capture accurate patient responsibility before the patient arrives.
This is what actually solves the problem.
Option 3: predictive eligibility with coverage change alerts
In addition to verification, the system tracks coverage changes. If a patient’s plan is changing in 30 days, the system alerts you. If deductibles reset, the system updates automatically. If authorization requirements change for common procedures, you’re notified.
Use case: You want to not just fix eligibility errors, but predict and prevent them.
The question is: which one do you actually need?
Most hospitals in “survival mode” (high denial rates, squeezed margins) need Option 2. It solves the immediate problem. Option 3 is a luxury for proactive optimization.
How to evaluate a vendor
Don't just ask about eligibility verification features. Ask:
Do they connect to real payer systems?
Some "eligibility verification" tools actually just check a cached database that updates once per day. That's useless for real-time verification. You need a vendor who connects directly to payer systems (or through a robust intermediary platform that does). Ask: "Do you connect directly to payer systems, or do you use a third-party clearinghouse?" If they use a clearinghouse, ask how often data is updated. If it's not real-time, it won't solve your problem.
What's their payer coverage?
They should have mapping for 500+ payers. Innobot has 800+ payers already mapped. If a vendor claims comprehensive coverage but only has 50-100 payers, you'll be doing manual verification for a huge chunk of your patient population.
Ask: "What payers do you cover for my state/region?" Get a specific list. Don't accept "most major players."
How fast is the verification?
Real-time eligibility checks should return in 3-10 seconds. If they're taking 30+ seconds, that's too slow for patient flow and creates bottlenecks at check-in.
How does the data integrate with your system?
The eligibility data needs to flow directly into your billing system, ideally automatically. If you're getting a spreadsheet report that you have to manually data-entry into your RCM system, the value collapses. You'll just be verifying faster but still making the same mistakes.
Ask: "How does eligibility data integrate with our EMR and billing system?" Ideally, the answer is "API integration that pushes verified coverage directly into your claim submission workflow."
What happens when they discover a coverage mismatch?
This is critical. If your system verifies coverage and discovers the patient's coverage is different than what you recorded, what happens? Does the system:
- Just log it and let your staff discover it later? (Useless)
- Immediately flag the discrepancy for a staff member to review? (Okay)
- Automatically correct the coverage information before the claim is submitted? (Good)
- Prevent the claim from being submitted until the discrepancy is resolved? (Best)
The best vendors don't just verify—they actively prevent mismatches from turning into claims.
What's their success rate?
Ask: "What percentage of your eligibility verifications are successful?" (Successful = returned usable coverage information). Innobot's automation success rate is 99.8%. If a vendor is claiming 95% or lower, that means 5%+ of verification attempts fail or return incomplete data. You'll still be doing manual verification on a significant chunk of claims.
What about failed verifications?
When automated verification fails (payer system down, invalid insurance info, etc.), what happens? Do they:
- Route to manual verification? (That adds 30+ minutes)
- Allow the claim to proceed with partial information? (That creates risk)
- Queue for staff review? (At least there's a human checkpoint)
Ask specifically: "When automated eligibility verification fails, what's your protocol?" The answer matters because failed verifications will happen—you need to understand the backup process.
How to implement without destroying your workflow
If you decide to implement automated eligibility verification, here’s how to do it without chaos:
Phase 1: start with pre-registration (weeks 1-2)
Don’t try to automate everything at once. Start with pre-registration eligibility checks. When a patient calls to schedule or books online, automated verification runs in the background. It captures coverage info and flags any issues before the appointment.
Why start here? Because pre-registration is low-risk. If something goes wrong, you have days to fix it before the patient arrives. It’s not like trying to verify coverage at check-in when there’s a line of patients waiting.
Success metric: 95%+ of pre-registered patients have verified coverage 24 hours before their appointment.
Phase 2: add check-in verification (weeks 3-4)
Once pre-registration automation is running smoothly, add check-in eligibility verification. When the patient checks in, the system reverifies coverage (because it may have changed since pre-registration). Front desk staff see coverage status and can ask patients about plan changes.
This phase is more complex because it touches your patient flow. But by this point, your staff understands the tool and the workflow. The confusion is minimal.
Success metric: 98%+ of check-in verifications complete in <10 seconds (don’t slow down patient flow).
Phase 3: integrate with claim submission (weeks 5-8)
Once pre-registration and check-in are solid, integrate eligibility verification into your claim submission workflow. Before a claim goes out, the system reverifies coverage one more time. If anything has changed, the system alerts the biller before submission.
This is the phase that actually eliminates eligibility denials. It’s also the most complex phase because it touches your billing workflow.
Timeline: A good implementation partner will have you live on all three phases within 6-8 weeks. (Innobot’s implementation timeline is 6-8 weeks, which is fast because it includes real transition planning, not just a cutover.) If someone promises faster, they’re cutting corners.
The staffing question: do i lose jobs?
This is always the question. “If we automate eligibility verification, what happens to our verification staff?”
Honest answer: their job changes, but you don’t have to let them go.
Currently, your verification staff are doing three things:
- Manually calling insurance companies to verify coverage (30-40% of their time)
- Data entry (entering verified coverage into your system) (20-30%)
- Troubleshooting coverage mismatches (30-40%)
When you automate verification, #1 and #2 disappear. But #3 expands. In fact, automated verification creates MORE troubleshooting work because you’re now catching mismatches in real-time instead of after denials occur.
Your verification staff transition to:
- Reviewing coverage discrepancies flagged by the automated system (they’re now a quality control function, not data entry)
- Handling exceptions (the 1-2% of verifications that the automation can’t resolve)
- Doing strategic coverage analysis (understanding your denial patterns and payer contract issues)
The headcount might drop 20-30% (you don’t need as many people doing routine verification), but you don’t have layoffs. You have redeployment.
Where do they go? They become denial analysts. Your authorization specialists. Your payer relationship management team. These are more valuable roles that directly impact revenue.
The hospital that fully automates eligibility verification and then retrains verification staff as denial prevention specialists will have significantly better revenue cycle outcomes than the hospital that keeps doing manual verification.
Key Takeaways
- Insurance eligibility verification errors are silently costing most mid-market hospitals $2-4M annually in preventable denials and rework.
- Common errors include: coverage lapses between verification and claim submission, missing authorization requirements, wrong payer information, and data entry mistakes from manual verification.
- Manual verification is slow (15-20 checks per hour), error-prone, and creates duplicative work. Hiring more staff doesn’t fix the underlying problem.
- Automated eligibility verification checks coverage in real-time against actual payer systems, captures complete coverage information, and can be executed at multiple touchpoints (pre-registration, check-in, submission).
- Hospitals implementing automated eligibility typically see 15-25% reduction in eligibility-related denials, 2-4 point improvement in clean claim rate, and 3-5 day DSO reduction within 3 months.
- Choosing the right vendor matters. You need: real-time connections to payer systems, 500+ payer coverage, fast response times, direct API integration with your billing system, and 99%+ automation success rate.
- Implementation takes 6-8 weeks if done thoughtfully (phased approach: pre-registration, then check-in, then claim submission). Anyone promising faster is cutting corners.
- Staff transition from manual verification to higher-value roles (denial analysis, authorization management, payer relationships) rather than layoffs.
Conclusion
Eligibility-related denials are one of the most expensive, and preventable, sources of revenue leakage when they occur at scale. The path forward starts with visibility. Measure your baseline by analyzing recent denial data, calculate the true financial impact of eligibility failures, and evaluate vendors through a focused lens that prioritizes payer coverage, real-time connectivity, integration, and proven implementation outcomes.
If you want to go deeper into automated eligibility verification, our guide on insurance eligibility verification software breaks down what to look for, how vendors differ, and what successful implementations typically deliver. You can also explore how Innobot approaches automated eligibility verification—our 99.8% automation success rate and 6–8 week implementation timeline are the result of solving RCM-specific challenges, not offering generic eligibility tools.
The right time to fix eligibility verification errors is when you recognize them as a systemic issue, not a series of one-off problems. Be precise about your baseline, measure improvement consistently, and hold your vendor accountable. You’ll know the solution is working when your billing team stops spending 30% of their time correcting coverage mismatches and starts focusing on higher-value denial analysis instead.
Ready to reduce eligibility denials and recover lost revenue? Contact us to discuss your current eligibility challenges and see how automation can make a measurable difference.


