Executive Summary
You’re at your desk at 6 PM on a Friday, staring at a 120-day aged AR report with $2.8M sitting in pending status. Your staff—all 23 FTEs in the billing department—have been running the same worklist approach for three years. They’re burned out. Your clean claim rate is 87%, which is… fine? Respectable, even. But you know it should be 95%+. You suspect there are denial patterns you’re missing because your team is too busy with manual data entry to actually think about root causes.
That’s when the question hits: Should we outsource revenue cycle management?
It’s not a new question. But it’s the wrong question, framed the wrong way. The real question is: When does outsourcing revenue cycle management actually solve the problem you’re facing—and when does it just trade one headache for another?
This article is for revenue cycle leaders who’ve already learned that no vendor can fix poor processes with a better interface. You need a framework.
Hook
You’re at your desk at 6 PM on a Friday, staring at a 120-day aged AR report with $2.8M sitting in pending status. Your staff—all 23 FTEs in the billing department—have been running the same worklist approach for three years. They’re burned out. Your clean claim rate is 87%, which is… fine? Respectable, even. But you know it should be 95%+. You suspect there are denial patterns you’re missing because your team is too busy with manual data entry to actually think about root causes.
That’s when the question hits: Should we outsource revenue cycle management?
It’s not a new question. But it’s the wrong question, framed the wrong way. The real question is: When does outsourcing revenue cycle management actually solve the problem you’re facing—and when does it just trade one headache for another?
This article is for revenue cycle leaders who’ve already learned that no vendor can fix poor processes with a better interface. You need a framework.
The Real Cost of Keeping RCM In-House (When You Shouldn’t)
Let’s be clear: there’s nothing inherently wrong with in-house revenue cycle management. Plenty of health systems run high-performing, efficient billing operations with internal teams. But there’s a specific scenario where in-house RCM becomes a silent profit drain, and most executives don’t see it coming until it’s too late.
The Math That Nobody Talks About
A billing specialist in a mid-market hospital costs you about $55K-$65K in salary, plus 30% benefits and overhead. That’s roughly $73K per FTE per year. With that $73K, you get:
- About 1,900 billable hours annually (after PTO, training, etc.)
- At an average throughput of 15-20 claims per hour, that’s roughly 28,500-38,000 claims processed
- But here’s the catch: that math assumes 100% focused work. In reality? You’re looking at 65-75% actual utilization due to system downtime, learning curves, and the fact that claim processing is cognitively draining work
So your real cost-per-claim is somewhere between $1.90-$2.73, depending on your staff’s experience level.
Now add the hidden costs:
- Turnover drag: Billing department turnover in healthcare averages 28% annually. When someone leaves, you lose institutional knowledge about payer quirks, timely filing deadlines, and the local insurance landscape. Retraining a new hire takes 6-8 weeks before they’re productive
- Compliance and training: Your billing team needs ongoing education on coding changes, ICD-10 updates, payer policy shifts. That’s not free
- System costs: Don’t forget EMR integration, billing software licensing, claims submission platforms, and the IT overhead of maintaining these systems
- Management overhead: Your RCM director is spending 30-40% of their time on people management, turnover, and process firefighting instead of strategy
For a hospital with 1,000-2,000 beds processing 80,000-150,000 claims annually, these hidden costs easily add another 20-35% to your baseline labor spend.
What You’re Actually Trading Away
Here’s what I see most executives miss: when you keep RCM in-house but your margins are tight (under 3%), you’re not really saving money. You’re just spreading the pain.
You’re paying for:
- A team that’s perpetually overwhelmed
- Quality escaping through the cracks (denials you don’t catch because you’re too busy processing volume)
- Innovation that never happens (your team is too busy firefighting to redesign workflows)
- Strategic revenue cycle insight that gets buried in day-to-day execution
The CFO sees “low cost per claim” and thinks that’s a win. The reality? You’re optimizing for the wrong metric.
What Most Providers Try First (And Why It Usually Fails)
Before we talk about outsourcing, let’s acknowledge what most hospitals try when they realize something’s broken:
Option 1: Hire more staff
This almost never works. If your processes are inefficient, adding headcount just scales the inefficiency. You’re hiring people to do busy work faster. Within 6 months, you’ll have hired 3-4 new people, burned through another $250K, and your clean claim rate still hasn’t moved. Worse, you’ve added management complexity.
Option 2: Implement new software
The vendor promises their RCM platform will transform your operation. Cleaner data! Better workflows! AI-powered denial prevention! (They mean rule-based alerts.)
Here’s what actually happens: you spend 4-6 months in implementation. Your existing team is already drowning, so they can’t dedicate cycles to configuration. The vendor assigns you a “project manager” who’s never worked in a hospital system with your revenue mix. You go live 2 months late. The software works fine, but your processes are the same—they’re just now documented in a new system. Your problems were never the software.
Option 3: Hire a consultant to “optimize” your RCM operation
A Big 4 consulting firm comes in, spends $150K on a 12-week engagement, creates a beautiful PowerPoint deck with 47 recommendations, and leaves. Your team doesn’t have bandwidth to implement 47 things. You implement 6. Nothing meaningfully changes because the real problem—understaffing and outdated workflows—is still there.
These three options have one thing in common: they assume the problem is operational (better people, better software, better processes). But sometimes the problem is structural. Your in-house team, no matter how skilled, can’t do claims processing and denial management and payer relationship management and denial write-off decisions and compliance monitoring with the same headcount.
That’s when outsourcing starts to make sense.
In-House vs Outsourced RCM: The Real Trade-Offs
Before we go further, let’s acknowledge something: outsourcing is not a panacea, and it’s not right for every health system.
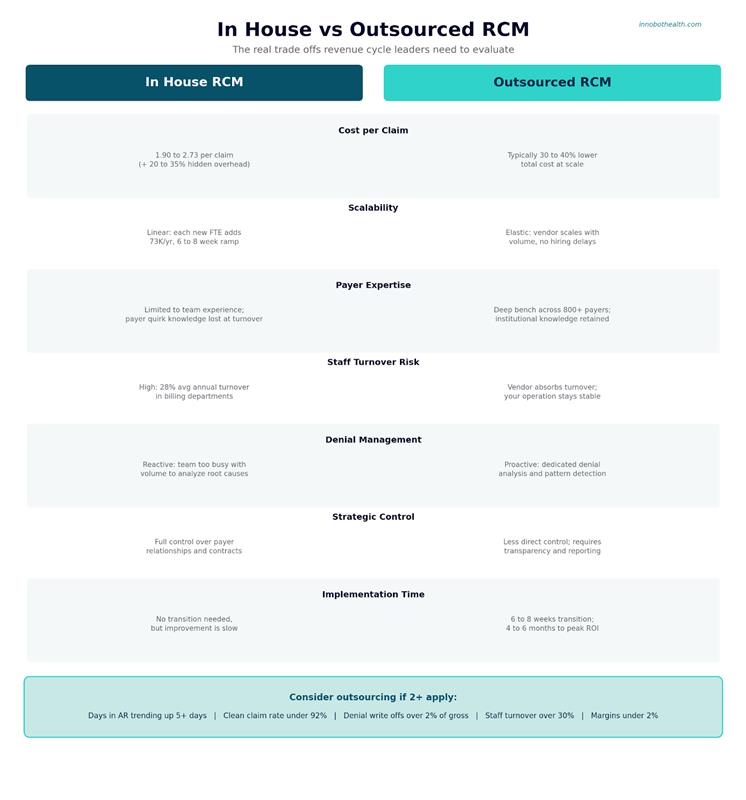
When In-House RCM Still Wins
Keep revenue cycle in-house if:
- You have complex, non-standard revenue streams: If 30%+ of your revenue comes from workers’ compensation, personal injury claims, or other non-standard insurance, outsourcing becomes messier. Third-party processors aren’t set up for these edge cases
- Your margins are healthy (4%+ net revenue): If you can afford 8-10 FTEs for a mid-market hospital and you like your team, there’s no urgent economic reason to outsource
- You view RCM as strategic: If your CFO or COO is genuinely engaged in denial trends, payer contracts, and revenue cycle metrics, they’ll be frustrated by outsourcing’s black-box nature
- You have a specific organizational reason to keep it in-house: Some health systems use RCM staff as a pipeline to train future hospital operations leaders. That’s a valid strategic choice
When Outsourcing Actually Makes Sense
Consider outsourcing if you hit 2+ of these markers:
- Your days in AR is trending upward (particularly if it’s moved 5+ days higher in the last 18 months)
- Clean claim rate is under 92% and your team can’t identify why
- Denial write-offs are eating >2% of gross revenue (that’s real money slipping away)
- Your team turnover exceeds 30% in the last 12 months (you’ve lost continuity)
- You’re manually reworking >10% of claims because they rejected or denied
- Your RCM team can’t prioritize denial analysis because they’re too busy with posting and worklist management
If you’re in “survival mode” (margins <2%) and any two of those are true, outsourcing isn’t optional, it’s necessary.
Medical Billing Denial Management Software: Why It Alone Isn’t Enough
Here’s where I’ll be contrarian: most health systems think the problem can be solved with better software.
They implement medical billing denial management software that promises intelligent denial prevention, automated worklist prioritization, and predictive analytics. The software is fine. Some of it is quite good.
But here’s what software can’t do:
- Make payer relationship decisions: When Blue Cross starts blanket denying knee replacements with certain diagnosis code combinations, that’s not a software problem. That’s a payer contract problem that requires someone on your side calling the payer and saying “we’re escalating this.” Software can flag it. A person has to own the relationship
- Handle exceptions at scale: You’ll have 2-3% of claims that hit weird edge cases—unusual insurance arrangements, third-party liability scenarios, coordination of benefits nightmares. Software will fail on these. A human needs to triage
- Perform strategic write-off decisions: When you have a $15K denial and the patient’s insurance actually was secondary but your EOB posting process missed it, that’s a judgment call. Do you reprocess and dig into 6 months of historic claims for the same issue? Or take a loss? Software can’t decide that. The revenue cycle director has to
So denial management software is a necessary component of outsourcing, but it’s not sufficient.
The Outsourcing Decision Framework
If you’re seriously considering outsourcing revenue cycle management, use this framework:
Step 1: Define Your “Must-Have” Outcomes (Not Preferences)
What does success look like for you? Write down 3-4 must-haves:
- “Clean claim rate of 94%+ within 6 months”
- “Days in AR under 40 by month 9”
- “Denial write-offs drop below 1.2% of gross revenue”
- “We maintain visibility into aging claims and denial trends”
Be specific. “Improved efficiency” is not a must-have. “Process $150K more in revenue per month with the same staff” is.
Step 2: Assess Your “Readiness”
Not every health system is ready to outsource. Before you even talk to vendors, ask yourself:
- Do we have clean, auditable data in our existing system? (Garbage in = garbage out)
- Do we understand our current revenue cycle metrics? (If you don’t know your baseline clean claim rate, you can’t measure improvement)
- Do we have executive alignment? (If the CMO thinks outsourcing is “losing control of quality” but the CFO wants it for cost, this will fail)
- Can we tolerate a 4-6 week transition period where everything is slower before it gets faster? (Most health systems can’t, which is why outsourcing implementations stall)
If you answered “no” to two or more, you’re not ready. Fix those first.
Step 3: Evaluate the Right Vendor Criteria
Forget the glossy case studies. Ask these questions:
Do they understand YOUR revenue mix?
- If you’re a cancer center with 60% commercial insurance, they better know that Blue Cross Anthem contracts are where your denials live
- If you’re a rural critical access hospital, they better understand Medicare Advantage quirks
- Ask for 3 references from hospitals with similar payer mix
What’s their actual timeline to productivity?
- Industry standard claims: 8-12 weeks to 85% automation; 4-6 months to 95%+ productivity
- Anyone promising faster is overselling or cutting corners
- Innobot’s 6-8 week implementation timeline is genuinely fast—ask why, and verify it with their references
How do they handle exceptions?
- They should have a clear escalation path for claims that require judgment
- Ask: “What percentage of claims require human review at your operation?” (Healthy answer: 3-5%. If they say <1%, they’re cutting corners and dumping problems back on you)
What visibility do you get?
- Daily reporting on processed claims, denials, AR aging
- Weekly denial analysis with root cause trending
- Monthly strategic review with your team
- If the vendor offers a quarterly report and that’s it, you’re outsourcing into a black box
Step 4: Understand the Failure Modes
Every outsourcing relationship has failure modes. Know them:
- The “volume dump” failure: Vendor accepts your entire workload, cuts corners on quality, clears the backlog fast, and leaves you with 5% higher denials
- The “transition hell” failure: You go live and for 3 months nothing works, patient statements are delayed, and your phones ring with angry billing inquiries
- The “knowledge loss” failure: You offshore your RCM knowledge to a vendor who doesn’t understand your payer relationships, market, or contracts
- The “cost creep” failure: Vendor starts at a good price point, then adds “exception handling” fees, “escalation fees,” and “advisory fees” until it costs 20% more than in-house
The best outsourcing partners are explicit about these risks and build guardrails against them.
What to Look For in an Outsourcing Partner
You need a partner who:
Speak your language: They know what a UB04 is. They know timely filing requirements. They understand the difference between a claim rejection and a denial. They won’t say “agentic AI” when they mean “a bot that makes decisions.” (This is why I started this article talking about days in AR and clean claim rates—because those are the metrics that matter to you)
Has operational depth: The people touching your claims should be revenue cycle professionals, not general offshore staff. Innobot brings 28 years of RCM experience from the founder level down through the operation. That matters.
Has already solved your specific problems: Ask to talk to 3 current clients with similar revenue profiles. Ask them directly: “Did they hit the timelines they promised? Did the software work as advertised? Did you see the ROI?”
Provides transparency: You should have real-time dashboards showing what’s being processed, what’s pending, what’s aging. You should have weekly or bi-weekly cadence reviews. You should feel like you’re still in control, just with better execution
Handle the transition thoughtfully: A good partner doesn’t just take over. They spend 4-6 weeks mapping your payers, understanding your contracts, and training on your specific workflows. That’s why Innobot’s 6-8 week implementation is actually feasible—it includes real transition work, not just a cutover
The Numbers: What You Should Expect
If you’re in “survival mode” with poor margins:
- Month 1-2: Transition period. Things might get slightly slower before they get faster. Don’t panic
- Month 3-4: Clean claim rate starts improving (target: +2-3 percentage points)
- Month 4-6: Days in AR drops noticeably (target: 5-8 day reduction)
- Month 6-12: You see sustained improvements. Denial write-offs shrink. Cash flow improves
Real example: Aqua Derm automated 380,000+ eligibility checks with Innobot, recovered $1.16M in 6 months, and freed up 46,000 hours of staff time. That’s not hypothetical. That’s operational improvement.
Is outsourcing an overnight fix? No. Can it cut your RCM overhead by 30-40% while improving your clean claim rate? Absolutely—if you pick the right partner and set it up right.
Key Takeaways
- In-house RCM works fine if margins are healthy and your team is stable. Outsourcing is optional in that scenario
- If you’re in survival mode (margins <2%) or your team is burning out, outsourcing deserves serious consideration
- The real question isn’t “in-house vs outsourced.” It’s “can we handle our current volume with our current headcount and still improve quality?” If the answer is no, you need to change something
- Software alone won’t fix RCM problems. Even robust automated denial management solutions are necessary but not sufficient without process redesign, payer strategy, and experienced operational oversight.
- Expect 6-8 weeks of implementation, 4-6 months to see peak improvements, and ongoing partnership for strategic optimization
- Pick a partner who speaks your language and has operational depth, not vendor polish. Ask about payer relationships, timely filing, UB04 requirements, and clean claim metrics—not “AI capability”
Conclusion
Outsourcing revenue cycle management only works when it’s done with intention. Start by grounding the decision in data, know your current days in AR, clean claim rate, and denial write-offs so you have a clear baseline. Define the specific outcomes you need, then evaluate partners who specialize in RCM and can speak confidently about payer relationships, transition timelines, and accountability.
If you want to see what a structured approach looks like in practice, Innobot’s guide to revenue cycle management services outlines the methodology, timeline, and results you should expect from a true RCM partner.
The right time to outsource isn’t driven by a vague goal to “be more efficient.” It’s when you’re solving a clearly defined problem, measuring progress against real metrics, and holding your partner to those expectations. When it works, the change is obvious—your team stops working late just to keep up and starts focusing on denial trends, optimization, and strategic improvement instead.
Ready to take the next step? Contact us to discuss your current challenges and see whether outsourcing RCM is the right move for your organization.


