Executive Summary
It’s 7:15 AM, and your revenue cycle director walks into your office with the daily denial report. You already know what it says: 1,200 claims denied yesterday. Not appealing. Not pending. Denied. Most of them hit the same five or six denial codes you see every single month.
You know what the biggest ones are, probably CARC codes 155 (Not covered by this payer), 96 (Referral/authorization unavailable), or 4 (Procedure code inconsistent with modifier). You’ve been staring at these denial codes for so long they feel personal.
Hook: The $47,000 Morning
It’s 7:15 AM, and your revenue cycle director walks into your office with the daily denial report. You already know what it says: 1,200 claims denied yesterday. Not appealing. Not pending. Denied. Most of them hit the same five or six denial codes you see every single month.
You know what the biggest ones are, probably CARC codes 155 (Not covered by this payer), 96 (Referral/authorization unavailable), or 4 (Procedure code inconsistent with modifier). You’ve been staring at these denial codes for so long they feel personal.
Here’s the thing: You’ve got the best billing staff in the region. But even with strong processes, medical billing denial codes are costing your organization hundreds of thousands every year, not just in lost revenue, but in the labor hours it takes to dispute them, resubmit, and track appeals that disappear into the payer’s black hole.
This article breaks down why these codes exist, why they refuse to die despite your best efforts, and what actually works to resolve them at scale.
Many organizations try to solve this by investing in denial management software, but most tools only organize denials after they happen instead of preventing them upstream.
Key Takeaways
- The top 5 denial codes account for 60-70% of all denials at mid-market health systems
- Most common causes are preventable with proper eligibility verification, prior authorization, and claim formatting before submission
- Manual appeal workflows can take 30-90 days; automation reduces resolution time to 7-14 days
- A mid-market hospital can recover $1.2-$2.8M annually by automating denial identification and routing
- 800+ payers now have standardized code mapping, making automation faster to implement
The Real Cost of Denial Codes You Can’t See
Let’s talk about the math nobody wants to admit.
Your average claim value is probably somewhere between $800-$1,500. When a claim gets denied, you’re not just losing that one claim, you’re losing the time it takes to:
1. Identify why it was denied (someone has to READ that EOB)
2. Determine if it’s appealable or if it’s a clean miss on your side
3. Route it to the right department (billing, authorizations, coding, or appeals)
4. Pull the clinical and financial records to support the appeal
5. Draft the appeal letter with supporting documentation
6. Submit and wait 30-90 days for a response
7. Post the secondary EOB if appealed successfully
8. Write it off if the appeal fails
Your billing staff probably spends 15-25 minutes per denial just on steps 1-3. Multiply that across thousands of denials per month, and you’re looking at 800-2,000 hours of labor annually spent on triage alone.
At $35/hour fully loaded, that’s $28,000-$70,000 per year, and that’s before you add the cost of appeals specialists, follow-up calls, and the ones that just… fall through the cracks.
But the real damage is the days in accounts receivable (AR). When denials languish for 60-90 days waiting for an appeal decision, those are dollars that should have been in your account 45 days ago. For a mid-market system processing $400M in annual revenue, every day of AR delay costs you roughly $1.1M in cash flow you could be using elsewhere.
The Five Denial Codes That Keep You Up at Night
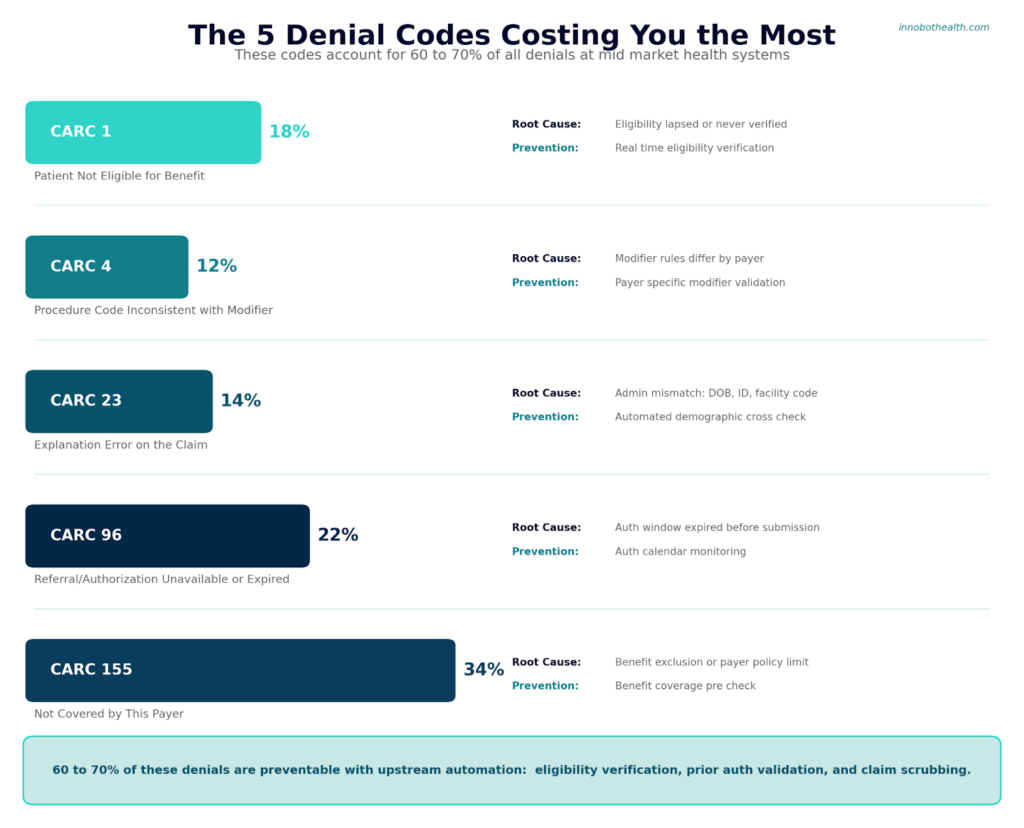
Not all denial codes are created equal. Some are one-time mistakes. Others are systemic problems that indicate a deeper process failure.
Here are the ones that show up on every denial report:
CARC 155: Not Covered by This Payer
This is the denial code that makes clinicians crazy. The service was clinically appropriate, the documentation is solid, but the payer says they don’t cover it.
Why it happens: Either the service genuinely isn’t a covered benefit (in which case it’s patient responsibility), or the payer is denying on the basis of a limitation they don’t advertise clearly. Blue Cross plans, for example, notoriously blanket-deny certain orthopedic procedures (like knee replacements) when the diagnosis code falls within specific ranges, not because the procedure isn’t covered, but because they use diagnosis-based exclusions that don’t always make clinical sense.
What most people try: Manual appeal with clinical justification. Sometimes it works. Usually it doesn’t, because you’re arguing policy, not clinical necessity.
CARC 96: Referral/Authorization Unavailable or Referral Expired
This one usually means you submitted the claim without the required prior authorization, or the auth you had expired between the auth date and the claim submission date.
Why it happens: Timeliness is brutal. Authorization windows are often 30 or 60 days. If your scheduling is backlogged, or if the patient reschedules, the author can age out before the claim ever gets submitted. And if you’re submitting claims on a batch schedule (which most systems still do), you might not catch the expired auth until the EOB comes back.
What most people try: Re-authorize and resubmit. If the service is still timely. If not, write it off.
CARC 4: Procedure Code Inconsistent with Modifier Used
Translation: You billed the procedure with a modifier that doesn’t match the payer’s rules for that specific code.
Why it happens: Modifiers are payer-specific. The same procedure with the same modifier might be billable to Medicare but not to United. Or it might require a different modifier on the same payer. Your billing staff memorizes the big three or four, but when you’ve got 15 players in your network, someone’s going to get a modifier wrong.
What most people try: Resubmit with the correct modifier. But by then, 45 days have passed.
CARC 23: Explanation Error on the Claim
This usually means some administrative detail on the claim doesn’t match the payer’s records, wrong patient DOB, mismatched subscriber ID format, or a typo in the facility code.
Why it happens: Most systems still do a lot of manual data entry, or they’re pulling eligibility data that’s old. The payer updated the patient’s record in their system, but you didn’t. Now you’re submitting against outdated information.
What most people try: Verify eligibility (again) and resubmit. But this often cycles through 2-3 times before someone catches what actually changed.
CARC 1: Submitted Charge Not Covered Under Plan/Patient Not Eligible for Benefit
This is different from 155. This usually means the patient’s eligibility was never verified, or it lapsed between the service date and the claim submission date.
Why it happens: Real-time eligibility verification would catch this, but most systems do batch eligibility checks or check it manually at the point of service, and then the patient’s eligibility changes before you submit the claim. Or, the patient is covered, but a specific service line isn’t covered under their plan (e.g., infertility services are excluded, or speech therapy has a limited number of visits).
Why Your Current Denial Management Process Isn’t Working (And Why It Can’t)
Here’s the hard truth: Manual denial management doesn’t scale. And it can’t, because of how denials actually work.
Your team can be incredibly sharp and still lose to volume. A mid-market hospital might receive 3,000-5,000 claim denials per month. Even if your billing team processes them quickly, they’re making decisions in a vacuum. A denial that looks like a one-time payer mistake might actually be a pattern that applies to hundreds of other claims currently in your AR.
Example: Blue Cross denies three knee replacement claims with CARC 155. Your team appeals to all three individually. Two get overturned, one doesn’t. But meanwhile, your system has 47 other knee replacement claims in AR with the same diagnosis code that haven’t been denied yet—they’re just sitting there, vulnerable to the same denial pattern.
Manual workflows can’t see that pattern until it’s too late.
On top of that, your denial management process is probably reactive, not preventive. You find out a claim was denied when the EOB comes back, sometimes 15-30 days after the claim was submitted. By then, it’s too late to catch preventable errors on similar claims. You’re fighting a problem after it’s already cost you money.
What Most People Try (And Why It Fails)
1. Hiring More Billing Staff
This is the first instinct. If denials are piling up, add headcount. But the math doesn’t work. You’d need to hire roughly one FTE for every 8,000-10,000 monthly denials just to keep up with triage. That’s expensive, and it doesn’t fix the root cause, you’re still reactive, still manual, still slow.
2. Implementing a Denial Management Software Solution (the Old Way)
Most legacy denial management platforms do what they call “denial workflow automation.” What that actually means: They collect denials from your EOBs, categorize them by denial code, and route them to the right team member’s inbox.
That’s useful, sure. But it’s not actually solving denials. You still need a human to read the EOB, determine next steps, and take action. You’ve just added a layer of organization on top of the same manual process. It might save you 10-15% of your denial labor, but you’re not touching the root causes.
3. Hardening Your Front-End Billing Process
This is better. You implement strict eligibility verification rules, add pre-claim validation checks, and maybe hire an authorizations specialist to babysit the prior auth calendar.
This absolutely helps. But it’s also assuming your team will never miss anything. The reality is that payer policy is constantly changing, and there are always edge cases. Your billing staff can’t memorize every payer’s rules for every procedure with every combination of modifiers.
4. Working with RCM Consulting to “Optimize” Your Denial Appeals Process
This is the “do more with what you have” approach. A consulting firm comes in, trains your team on appeal best practices, and maybe identifies a few systematic issues. You implement some of their recommendations, and your appeal success rate goes from 35% to 42%.
That’s good! But it doesn’t prevent the denials in the first place, and it doesn’t speed up the resolution timeline. You’re still taking 60-90 days to get paid on appealed claims.
Traditional denial management services often focus on appeals and follow-ups, but they rarely address the systemic causes driving recurring denial codes.
Why These Approaches Miss the Mark
They all treat denial management as a people problem, when it’s really a data problem. Your team isn’t the bottleneck. The bottleneck is that you don’t have real-time visibility into payer denials patterns across your entire claims inventory, and you can’t act on that visibility fast enough.
A Better Framework: Prevention + Intelligence + Speed
The real opportunity sits at the intersection of three things:
1. Prevention: Stop Denials Before They Happen
This means:
- Real-time eligibility verification that runs against multiple payers every time a claim is about to be submitted, not just at check-in
- Automated prior authorization verification that confirms the auth is valid, within the required window, and matches the claim being submitted
- Claim validation that checks modifiers, diagnosis codes, procedure codes, and patient demographics against payer-specific rules before the claim leaves your system
This isn’t magic. It’s straightforward automation that catches the 60-70% of denials that are preventable. Once you stop the bleeding on preventable denials, you can focus on the genuinely complex ones.
2. Intelligence: Understand Why Denials Happen (and What It Means)
When a denial does come back, you need to instantly:
- Categorize it accurately against the denial code and understand what the payer actually meant
- Determine next steps (is it appealable? Is it patient responsibility? Is it a payer error? Is it a pattern affecting multiple claims?)
- Identify systemic patterns (if one payer is denying a specific procedure, what other claims in your system are at risk for the same denial?)
This requires mapping your claims data against payer rules continuously, not just when EOBs come back.
3. Speed: Resolve Denials in Days, Not Months
Once you know what to do about a denial, you need to do it immediately. That means:
- Automated resubmission for denials that are just administrative errors (wrong modifier, typo in ID)
- Automated appeal generation that pulls the right supporting documentation and drafts the appeal letter
- Intelligent routing that sends complex denials to the right specialist with all the context they need, not just a line item in a queue
The combination of prevention, intelligence, and speed moves your denial resolution timeline from 60-90 days down to 7-14 days. And for denials that are actually preventable, they disappear entirely.
How Automation Actually Changes the Game
Let’s look at two real examples of how this plays out operationally.
Case Study 1: Surpass – Eligibility Verification at Scale
Surpass was spending hours every week manually verifying Medicaid eligibility for hundreds of patients across multiple states. Their team was logging in and out of various state Medicaid portals, tracking down information, and keying updates into their EHR. It was tedious, time-consuming, and completely pulling staff away from patient-facing work.
The Problem: Manual eligibility verification was a bottleneck. The team couldn’t keep up with the volume. As their patient population grew, the workload became unsustainable.
The Solution: Innobot built a custom module that automated Medicaid eligibility verification across six states. The module dynamically adapts to changing eligibility requirements and state-specific rules. Now, hundreds of patient eligibility checks are processed simultaneously, daily.
The Result: What used to take significant manual effort is now completed 95% faster. The module keeps pace with demand growth without adding headcount. The team redirected their focus to higher-value patient care instead of repetitive data entry.
Why this matters for denial prevention: This is prevention in action. When eligibility is verified in real time, eligibility-based denials simply don’t happen. You never submit claims for ineligible patients or during coverage gaps.
Case Study 2: Behavioral Health Works – From 4-5 Billers to 1
Behavioral Health Works, a billing and collections organization serving children with autism, had a team of four or five billers handling insurance eligibility checks, payment posting, and claim submission. The workload was heavy, checking insurance eligibility monthly was time-consuming, and posting payments across multiple payers with different formats was tedious.
The Problem: Labor cost was high, efficiency was low, and the team was burning out on repetitive tasks.
The Solution: Innobot automated their eligibility checking and payment posting workflows. The modules check insurance eligibility automatically and post payments from multiple payers without manual intervention.
The Result: They reduced their full-time billing staff from four or five to just one. That one person now uses the automation platform. The modules handle the volume. The hours previously spent on eligibility and posting were freed up entirely.
Why this matters for your CFO: This is direct cost reduction. Behavioral Health Works went from five FTE costs to one FTE plus software cost. The ROI on that redeployment is immediate, and it compounds, as their patient volume grows, the software scales without linear headcount growth.
The Operational Shift
Both of these examples show the same pattern: Prevention + Intelligence + Speed = Different Business Model
You’re not hiring more billers. You’re not training people on every payer’s rules. You’re not relying on human memory and spreadsheets.
You’re automating the preventable denials (eligibility, prior auth, formatting errors) so your team can focus on the genuinely complex appeals. You’re freeing up labor for high-value work. And you’re getting cash back faster.
Here’s what separates this from “workflow software” you’ve probably already tried: These aren’t just systems organizing denials after they happen. This is prevention, stopping denials before submission. That’s why the timeline is so different. You’re not spending 60-90 days on appeals for preventable denials. Those denials don’t exist.
What to Look For in a Denial Automation Solution
If you’re evaluating how to automate your denial management, here are the capabilities that actually matter:
Prevention-First Architecture
Does the solution check claims before they’re submitted, or does it only organize denials after they come back? Prevention-first means eligibility verification, prior auth validation, and claim scrubbing. Denial-organization means you’re still reactive.
Ask: “How many payers do you have in your real-time eligibility database?” (The answer should be 800+.) “Can you verify auth validity in real time?” “Do you validate modifiers against payer-specific rules?”
Payer Intelligence Without Manual Mapping
If the vendor is asking you to manually map denial codes or tell them about your payer contracts, they’re outsourcing the complexity to you. They should have deep payer intelligence built in—they should already know what CARC codes mean at each payer, what the appeal success rate is, and when an appeal isn’t worth pursuing.
Automation That Learns From Your Corrections
The system will never be perfect. But it should learn from corrections. If your team overrides an automated decision, the system should log that, identify patterns in your overrides, and adjust future decisions.
This is different from “machine learning” in the AI sense. This is pattern learning within your own operational context.
Integration, Not Replacement
Does it work with your existing billing system, or does it require a rip-and-replace? Good solutions integrate with your EHR and billing platform. They don’t ask you to move workflows out of your existing tools.
Realistic Speed and Implementation
If someone tells you they can implement denial automation in 2-4 weeks, they’re either overselling or they’re doing a light integration. Realistic timelines are 6-10 weeks, which includes:
- Understanding your current denial patterns
- Mapping your specific payer contracts
- Testing against your real claim data
- Training your team
- Going live with safety checks
Implementation: Where to Start
If you’re thinking about automating denial management, here’s a practical sequence:
Month 1: Audit Your Current State
Pull three months of denial data. Categorize it by denial code, payer, and root cause. You should find that 60-70% of your denials fall into 5-8 main categories. Those are your immediate targets.
Also calculate your current cost: How many hours does your team spend on denials per month? What’s your average day in AR on denied claims? What’s your appeal success rate? These become your baseline metrics.
Month 2: Identify Your Biggest Payer Pain Points
Which players are hitting you with the most denials? Which denial codes are costing you the most money? Focus there first.
If you’re getting 200+ monthly denials from one payer on the same code, that’s usually a process problem with that specific payer. That’s your first automation target.
Month 3: Pilot Prevention on Your Worst Category
Pick your highest-impact denial code and payer combination. Implement automated eligibility verification or prior auth validation for claims that match that profile. Run it in parallel with your current process for 2-4 weeks, measure the results, then flip the switch.
Ongoing: Measure and Expand
Once you’ve proven ROI on the pilot, scale to other denial categories and payers. You should see measurable improvements in:
- Percentage of preventable denials (should drop 60-80%)
- Days in AR on denied claims (should drop 50-70%)
- Appeal success rate on remaining denials (should increase 20-30%)
- Denial labor cost (should drop 40-50%)
The ROI: What to Expect
For a mid-market hospital ($100M-$1B in net patient revenue), automating denial management typically yields:
Direct Financial Recovery:
- Prevention of 500-1,200 denials per month (at $800-$1,500 per claim) = $400K-$1.8M annual recovery
- 20-30 day reduction in AR on appealed denials = improved cash flow (hard to quantify but operationally significant)
Labor Savings:
- Reduction in denial triage, appeals management, and resubmission hours = 600-1,600 hours annually (at $35-45/hour fully loaded) = $21K-$72K annual savings
Total Year 1 ROI: $420K-$1.87M
Implementation costs typically range from $60K-$150K depending on the breadth of integration. Most customers hit payback within 2-4 months.
What This Means for Your Strategy
If you’re a CFO or revenue cycle executive looking at this problem, the framing is important. This isn’t about “AI” or “cutting-edge technology.” It’s about moving from reactive, manual denial management to preventive, intelligent denial management.
Your team is probably already doing good work. What they’re missing isn’t effort, it’s visibility and automation. They can’t see patterns across 3,000-5,000 monthly denials. They can’t manually check every claim against every payer rule before submission. They can’t be in two places at once.
Automation fills that gap. And it’s not about replacing your team, it’s about redirecting them toward complex problem-solving instead of data entry.
Conclusion: The Cost of Waiting
Here’s what we know from working with 50+ mid-market health systems: The ones that move on denial automation first gain a competitive advantage.
It’s not because they’re more tech-forward. It’s because they’re putting cash back into their organization faster, freeing up labor for high-value work, and building institutional knowledge about what actually works with their payers.
The ones that wait? They usually rationalize it for 18-24 months. By the time they implement it, they’ve left millions on the table, not because they made a mistake, but because they deferred fixing a broken process.
Medical billing denial codes aren’t going away. Payers will keep denying claims, and some of those denials will be legitimate. But 60-70% of them are preventable. That’s not your team failing. That’s a systems problem, and systems problems have systems solutions.
The question isn’t whether to automate denial management. It’s when, and with how much of that $1.2-$2.8M recovery potential you’re willing to leave behind.
If you want to understand how much revenue denial automation could unlock in your organization, contact us to review your denial patterns and identify high-impact automation opportunities.


